Editors Note: Elizabeth was accepted into Georgetown University, and starts her freshman year this fall. She chose to write her college essay on her experience at the Clinic, and we wanted to share this with you as part of her wonderful Rumspringa blog. Congratulations, Elizabeth!
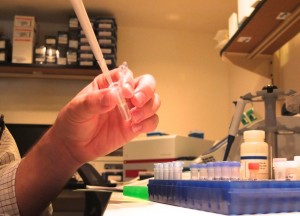
As I hold the test tube to the light, I see it: a tiny opaque ribbon, the size of a fingernail. Just an hour ago, this had been my blood. After pipetting chemical after chemical, pouring, mixing, shaking, and filtering, I now had my “little ribbon,” my DNA, which holds all the information of who I am and the potential for who I will be. At this moment, the spiral of my life is in my hands. And I know I am unique.
I came here to the backcountry of Strasburg, Pennsylvania to understand this individuality, not in a chemical sense, but rather in a communal one. Here lies the Clinic for Special Children, a pediatric practice serving the Amish and Mennonites. Erected, literally, in the middle of a cornfield, the Clinic is unique in using high-tech tools to discover the roots of genetic illnesses in patients who drive horses and buggies. I journeyed to the Clinic to get a taste of how special these children really are, whereupon I put myself in their shoes, testing my own DNA for the same genetic illnesses that they might have.
In the beginning, this opportunity seemed like a long shot. The Clinic has an internship program, however, it is limited to undergraduates and medical students. As a rising twelfth grader, I loved science and children. I wanted to experience what it is like to help in a medical setting. Thus, I created a plan to launch a social media campaign and drafted a proposal to raise awareness and money for the Clinic’s mission. I would shadow the doctors, work in the lab, meet the families, and soak up anything I could. With that information, I would create a blog, Facebook messages, and Instagram posts. The Clinic staff was intrigued. And there I was in the lab, testing my DNA.
From my “little ribbon,” I learned that I carry the genes for blue eyes, lactose tolerance, and a common mitochondrial mutation. I also discovered that I do not have a severe genetic condition called maple syrup urine disease, thank goodness. In the Clinic, I came to know the importance of cultural understanding and bedside manner, as pediatrician Dr. Kevin Strauss sleuthed and explained serious ailments to white-bonneted and suspender-clad patients. I also ventured out into the community. I ate pizza in the homes of three Amish families, rode in a pony cart along with Amish children, drank milk straight from a cow’s udder, and helped can peaches. 
These moments wove together to teach me the values of community and culture in relation to individuality. I come from the “Brookline, Massachusetts bubble,” where high school is a vehicle to jam-pack a resume by volunteering at soup kitchens, tutoring underprivileged children, or organizing bake sales to help African children buy goats. All of this check-marking has become so routine as to be commonplace. I wanted to break that mold.
I arrived hoping that the Clinic could help me step outside the bounds of my environment, which insists on excellence at any cost. The community welcomed me and made me feel more than excellent. I felt special. Now I know that whatever I do with my life, I will carry this feeling with me and, most importantly, create the means to offer it to others. I can say now that I want to foster a career in which I apply scientific knowledge and share it with others, while working with different cultures. Maybe I will incorporate art therapy into a clinical practice, serving minorities, or teach science to foreign students. I cannot predict the particulars, but I do know this: to be unique in Brookline language is to stand out, but to be special in Clinic terms is to join in, becoming one with something much larger – a community that values me for who I am and fits so tight that we achieve excellence together.






 l hyperplasia or CAH.
l hyperplasia or CAH. “There is no greater joy as a doctor and educator than to see bright young students interacting with the patients and families we serve, tackling complicated problems and building trust. We could not have asked for a better outcome for our students and families,” says Dr. Strauss.
“There is no greater joy as a doctor and educator than to see bright young students interacting with the patients and families we serve, tackling complicated problems and building trust. We could not have asked for a better outcome for our students and families,” says Dr. Strauss.

 al intensive care unit. Last summer, She was an intern at the Hershey Medical Center within the biochemistry department. Kendra is now finishing her coursework at F&M, including CSC’s “Plain People and Modern Medicine” capstone biology seminar.
al intensive care unit. Last summer, She was an intern at the Hershey Medical Center within the biochemistry department. Kendra is now finishing her coursework at F&M, including CSC’s “Plain People and Modern Medicine” capstone biology seminar.

 from the University of Georgia visited CSC for a family meeting about GM3 synthase deficiency, a devastating neurological disorder found in the Old Order Amish population.
from the University of Georgia visited CSC for a family meeting about GM3 synthase deficiency, a devastating neurological disorder found in the Old Order Amish population.